Gabriella Day is a GP, author and advocate of whole person medicine.
Gabriella Day is a GP, author and advocate of whole person medicine.
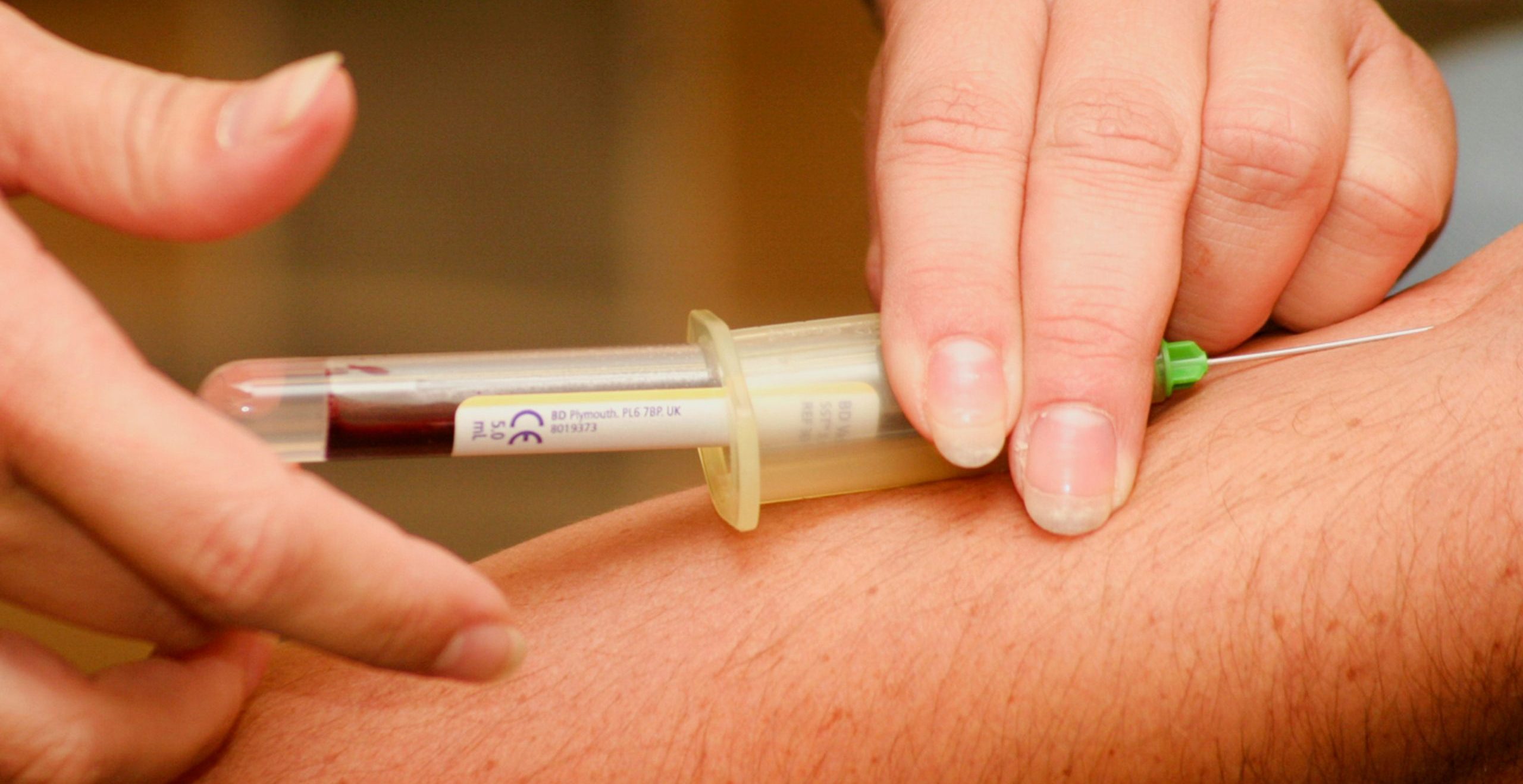
“L[/dropcaps]et’s just do some bloods…”
Are we seeing an increase in the instances where clinicians, apparently at a loss as to what else to do, just order some blood tests?
Why might we be ordering ‘bloods‘? If it helps elucidate a problem or excludes a significant and realistic underlying treatable cause, it is reasonable. Are we being honest with ourselves, however, or are we using it as a means to prevaricate, or kick the problem down the line?
The patient sees another clinician with the results. The first clinician has escaped without having to solve or progress the situation.
In my GP-training I was told, “Know what you’re doing.” This meant that if you’re investigating or referring, be mindful of why you are doing it.
We are now perhaps evidencing, “I think I know what it is, but I don’t know have an effective way of managing this.”
MRCGP taught us to choose a course of action that would help clarify the situation, in order to make a diagnosis and implement a management plan.
In the book, ‘I Don’t Know What it is, but I don’t think it’s serious’, Tim Crossley encourages us to acknowledge when we have done enough, because otherwise we are potentially going on to cause harm to the patient, condemning them to more and more tests and referrals with diminishing returns.1
There is increasing awareness of medically unexplained symptoms in general practice.2 Often, we may be aware that a patient’s pattern of presenting illness fits into one of the newer syndromes. Whilst becoming more well-recognised, this may still have limited treatment pathways to alleviate its impact.
We are now perhaps evidencing, “I think I know what it is, but I don’t know have an effective way of managing this.”
I wonder if there is a reluctance amongst clinicians to voice this.
What’s behind this reluctance? A fear of getting it wrong, of missing a cancer diagnosis, of the patient thinking us inadequate as clinicians when we have little to offer in terms of treatment? Fear that we will incur the wrath of the patient?
Of course, the likelihood of wrath being expressed increases as patients are pushed from pillar to post without any coherent explanation as to what might be causing their symptoms.
Uncertainty causes anxiety and fear, escalating pathology, frustration and emotional fragility.
It’s not kind to avoid proposing a ‘(dys)functional’ diagnosis for a patient or a diagnosis of a pathology for which we have limited treatment options; it carries considerable cost, financial, in escalating waiting lists and in leaving patients in limbo, unable to move forward with their lives in the face of uncertainty.
There is also a cost to the clinician. When we are adopting the ‘just get some bloods’ deferral and avoidance strategy, we are avoiding difficult conversations and covering up our lack of expertise. We then deny ourselves a learning opportunity. In the ‘ashram’ of general practice we are presented with the opportunities we need in order to grow, if we will see them as such.
Anyone can implement a protocol. Anyone can order a blood test.
The real skill of a primary care clinician is in navigating the complexity and finding a helpful path forward for the unique individual in front of us.
…the likelihood of wrath being expressed increases as patients are pushed from pillar to post without any coherent explanation as to what might be causing their symptoms.
To formulate even a tentative and provisional diagnosis is to start to find a way forward and help patients get their lives back on track.
We also then start to engage with and understand the amorphous mass of vague and indeterminate illness that is permeating all through society.
Then we can start to find better ways to manage it, ameliorate the impact on patients and society, perhaps even identify novel solutions to these complex and often life-changing illnesses. I don’t think these will be pharmaceutical solutions. I think they will involve us restoring practices that have been used for centuries and involve the quality of our physical, emotional and spiritual diets, reconnecting with the earth and ourselves in a way we have lost only in recent years.
We do our patients no favours through avoidance. And we do ourselves a disservice in avoiding the learning opportunities and the belief that when we engage with these new presentations, we can rise to the challenge of addressing them.
To tackle these issues is to help us find a way out of a quagmire, emerging as a more cohesive society.
Deputy Editor’s note – see also: https://bjgplife.com/when-normal-tests-end-care-too-early/
References
- Malterud K, Aamland A. Medically unexplained symptoms: are we making progress? Br J Gen Pract. 2019 Apr;69(681):164-165. doi: 10.3399/bjgp19X701885. PMID: 30923138; PMCID: PMC6428472.
Featured Photo by Hush Naidoo Jade Photography on Unsplash