
The Caravan of Hope
Myanmar (formerly known as Burma) has been a nation at the crossroads for more than ten years.1 The caravan of hope set off following the release of Aung San Suu Kyi in 2010, picking up speed after the release of political prisoners and the commencement of some democratic reforms in 2011. The journey out of darkness continued with visits from Hillary Clinton, USA Secretary of State, in 2011 and President Barack Obama in 2012. In 2015 Aung San Suu Kyi won a supermajority of the seats for the National League for Democracy (NLD) and a combined national parliament was formed with 25% predetermined seats for the military.
Her victory raised the hopes of the youth of the nation towards a brighter future. The onward journey has been bumpy with many setbacks under this fragile democratic arrangement. Despite these challenges, the NLD again won the parliamentary elections in November 2020 in a landslide victory. Then on the 1st February 2021 the Tatmadaw (the armed forces) blocked the road ahead and the caravan ground to a halt.
[Aung San Suu Kyi’s] victory raised the hopes of the youth of the nation towards a brighter future.
I clambered onboard this caravan in January 2018 when I made my first visit to Myanmar for the start of the RCGP – Myanmar GP Society Quality Improvement project. My fellow travellers were three colleagues, all UK GPs, two of whom were originally from Myanmar.
Of course you can’t just turn up and hitch a ride. Work to support the development of family medicine as a specialty had been going on since 2013 in close liaison with the Myanmar GP Society and the Myanmar Medical Association. Discussions had also been held with the Health Minister.
The Road to Mandalay
The project was to take place in the Mandalay region of Myanmar, in the city of Meiktila, population 150,000, and in Mandalay the second largest city in Myanmar, population 600,000, some 450 miles from Yangon. We could have taken the Yangon to Mandalay Expressway but we took the old road to Mandalay along with freight traffic that is not allowed on the Expressway. This was of course slower but offered a glimpse of towns, pagodas, local festivals, markets and other slices of life, including two wheel road haulage and bullock cart racing!
Stepping Out on The Road to Universal Healthcare
We were in Myanmar to support progress towards the recognition of General Practice as a specialty that would meet the challenges of developing UHC.This was to be a year long Quality Improvement (QI) project involving 64 practices in 16 Townships covering a population of approximately 2.5 million. 30% of practices were in urban areas, the rest were in small towns and large villages.
In Myanmar most GP surgeries are single-handed practitioners working in a small room with patients waiting outside. Many GPs work in professional isolation and there is no requirement for postgraduate qualifications or training in primary care. The majority of care provided in Myanmar GP practices are for acute episodes of illness, despite the burden of chronic diseases such as diabetes and hypertension. The majority of patients who see GPs as their first point of access to health care are the poorest people in Myanmar, this is especially so in rural areas. The better off usually access specialist healthcare directly. Continuing Medical Education (CME) is provided by secondary care, the topics and didactic style of teaching do not cater to a GP’s learning needs. Does this ring any bells for the state of General Practice in the UK in the years immediately preceding and following the birth of the NHS in 1948 (the same year that Burma regained independence)?
A New National Health Plan for Myanmar 2017 -21 was launched in March 2017 by Aung San Suu Kyi.2 The goal was Universal Healthcare (UHC) for the entire population of Myanmar by 2030. The foundation of this plan was to be primary care. However despite the importance of General Practice in the new National Health Plan, it was not recognised as a medical specialty. There was no comprehensive General Practice activity nor quality data. There are parallels here with early UK General Practice which was vital to the functioning of the new NHS but failing. In response to this the RCGP was founded in 1952 to support good standards of practice, education and research and develop General Practice as a specialty. In Myanmar The Quality Improvement Project was conceived and funded in response to their goal of UHC.
There are parallels here with early UK General Practice
The Quality Improvement (QI) Project
Just to remind ourselves, QI is about achieving best performance with the available resources. In the U.K. we have become familiar with methods that include audit, case review, significant event analysis and the identification of our learning needs through the appraisal process. But imagine hearing about this for the first time.
Data was collected on structure and process from all the GP practices at the commencement of the project and at the end. The RCGP Team visited GP practices to discuss and advise on quality indicators, professional / practice development (PDP), and to provide encouragement and moral support. Three days of workshops were carried out each lasting four hours, topics included the principles of Quality Improvement and the technical skills required . Lunch was included to accommodate the pattern of morning and evening surgeries seven days a week. Many of the doctors travelled a significant distance to attend.
The main areas for practice development were improving medical records, proper clinical waste disposal, and infection control, including hand washing and cleaning of premises. PDPs included plans to take the MRCGP International, targeted CME that was relevant to local GPs, and to learn about group practice. One of the desired outcomes of the one-year QI Project was that the GPs would continue to meet in small groups of 8-10 (Quality Circles) to learn together as a way of creating collaborative improvement in primary care.
Four visits to Myanmar by volunteer RCGP trainers were undertaken and six Myanmar GPs visited the UK at the end of the project to observe quality improvement in UK GP surgeries.
What Did We Find?
This was a rich and rewarding experience. The welcoming attitude of the GPs to new ideas and ways of learning was a major strength of the project. Group work was popular and the doctors were keen to contribute and share learning. Among the GPs in Mandalay and Meiktila who completed the RCGP QI Training we found significant improvement in infection control, and in medical records, which allowed 64% of doctors to carry out an audit of chronic disease management (CDM). 63% of doctors keep a record of their learning, and 70% have a PDP.3
100% of doctors who completed the training belong to Quality Circles, which have become an established method of collaborative learning. They have reduced professional isolation and increased the confidence to learn in peer groups. The shared development of medical records which included colour coding for CDM, the development of a register for CDM and the basic development of electronic medical records are a reminder of the pre-digital age in UK General Practice.
The Covid Pandemic
Digital technology came to the rescue when the Covid pandemic arrived in March 2020. The programme was adapted to remote working to ensure achievement of the long-term project objectives of improving quality in Myanmar General Practice, alongside the short-term objectives of preparing for COVID-19. The revised remote QI training programme included small group-training for those new to quality improvement, and small-group training to support graduates of the 2018 project to become Quality Champions, charged with promoting quality improvement within Myanmar. Additional elements included Webinars for GPs from all over Myanmar to facilitate sharing of learning and experiences during COVID and a Facebook Group between Myanmar and UK GPs. The necessity of remote teaching has had some advantages. Training in areas that are not geographically close has become possible. For example were due to start training in Sittwe the capital of the troubled Rakhine state, and Quality Champions from Mandalay and Meiktila have been involved in remote teaching of QI to GPs in other localities in Myanmar.
Other linked RCGP projects have included GPs trained as trainers; supporting the five non military universities of medicine in assessment techniques for use within their new integrated undergraduate curriculum, and the development of a new Masters degree in family medicine. Family medicine was arriving as a specialty in Myanmar.
The coup in the early hours of 1st February has halted all the progress made so far along the road to Universal Healthcare and the development of family medicine as a specialty in Myanmar.
The Nightmare
“All medical professionals including general practitioners and other health care workers in Myanmar should be able to deliver medical care to anyone in need of their help, without fear of intimidation, attack or arrest”.4
Human rights activists, and least of all the people of Myanmar, will not be surprised at the violation of medical neutrality in contravention of international humanitarian law.
Following the coup, Myanmar military and police forces have indiscriminately barraged crowds of peaceful demonstrators and volunteer medics with tear gas, rubber bullets and even military grade weapons. Scores of doctors, clearly distinguishable by the signature red cross on their clothes, have braved such dangers to treat injured protestors but have not been immune to the violence that sweeps Myanmar. Some doctors do not return to their homes at night.
The image of a medical student beaten unconscious by five helmeted men with truncheons, his apparently lifeless body dragged across the street, is a shocking distillation of the brutality and ‘otherness’ of the junta. If by chance he survived what medical care would be available?
We have clear photographic evidence from colleagues in Myanmar which shows a Doctor at gunpoint (above, right), a doctor arrested, destruction of a COVID centre and medical equipment taken away, a doctor’s request to complete suturing of an extensive head wound denied, civilians carrying injured patient on a wooden cart as an ambulance not allowed access (see the picture at the top of this article), paramedics from a charity clinic beaten, a paramedic trying to control severe bleeding from rubber bullet injury and the blood stained white coats of medical students after protest.
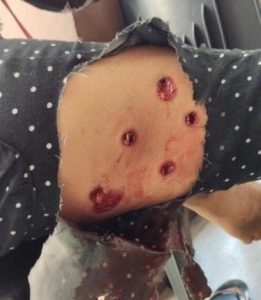 The information from Amnesty International is that the security forces in Myanmar are using shotguns loaded with rubber bullets (see left*), and the circumstances are that people are being shot at close range e.g. when fallen to the ground and surrounded by a group of the military. The intention appears to be to seriously harm, not simply disperse. This has been described by Amnesty as “contentious crowd control methods”. 5
The information from Amnesty International is that the security forces in Myanmar are using shotguns loaded with rubber bullets (see left*), and the circumstances are that people are being shot at close range e.g. when fallen to the ground and surrounded by a group of the military. The intention appears to be to seriously harm, not simply disperse. This has been described by Amnesty as “contentious crowd control methods”. 5The military and police forces occupy non-military hospitals and emergency services as their bases, life support machinery and equipment has been removed, facilities vandalised, and healthcare professionals threatened.
All of this is an attempt to undermine the civil disobedience movement. Doctors as citizens of Myanmar are balancing their right to protest against the coup with their public duty to provide medical care.
“Civil disobedience can be justified when used to protest a high stakes political decision that will affect many, not just for this generation but future generations”.6
Successive regimes in Myanmar have an appalling record on healthcare. Until the democratic reforms the spend on healthcare was less than 2% of GDP, under limited democracy that rose to 4.5%. The price of the coup, particularly in the midst of a pandemic will be the lives of ordinary people denied the healthcare that the military provides for its own.7
“Empathy is incomplete when it does not lead to action, an attempt to help”.8
Bearing witness, for our colleagues in Myanmar, as so many of us do for our patients, is powerful, but it is not enough. Colleagues in Myanmar want us to be their advocates, hear their stories, condemn the violation of medical neutrality, provide remote clinical guidance, especially on trauma medicine and communicate with them safely. It’s the least we can do.
What Next For Myanmar?
“We are writing this new chapter with our own hands”
Generation Z. Myanmar.
The protesters are not backing down, the street cannot easily be silenced. The impact of democracy over the last 10 years, however flawed, has diminished the suffocating influence of the junta.
The sunset in Myanmar from Inle Lake in the Shan Hills to the Shwedagon Pagoda in Yangon, is a natural masterpiece. Let us hope that the sun will rise on a new chapter of peace, democracy, prosperity and of course, universal healthcare for the people of this beautiful country.
References
- Rogers. B. Burma. A Nation at The Cross Roads’. Penguin Random House, [2015].
- Myanmar National Health Plan 2017 – 2021 Ministry of Health and Sports. mohs.gov.mm. [2017]
- RCGP Myanmar GP Society Quality Improvement Project Report. [September 2020.]
- Myanmar – UK GP Health Action. [March 2021]
- https://www.amnesty.org/en/latest/news/2021/03/myanmar-arsenal-troops-deployed-crackdown/ and personal communication
- Aung.S. Personal communication. [February 2021]
- Williams V.N. and Williams. T.I. Personal communication [March 2021]
- Coulehan.J.’“Let me see if I have this right”: Words that help build empathy’, Annals of Internal Medicine, Volume 135, p 221 [2001]
see also:
MYANMAR DOCTORS UNDER A MILITARY COUP IN THE MIDST OF THE PANDEMIC in BJGP Life,
and the Myanmar UK GP Health Action Group’s letter to the BMJ, which explains the endorsement by The Academy of Medical Royal Colleges:








[…] also THE DREAM OF UNIVERSAL HEALTHCARE IN MYANMAR BECOMES A NIGHTMARE in BJGP […]
Hay Mar Aung is from Myanmar. She currently works as an Emergency Medicine Registrar in the UK.
My country was trying to cultivate the tree of democracy and freedom when on the 1 February 2021 the military coup, justified by false claims of election fraud, took us back to the dark days of military rule.
Thousands of civilians went on strike and protested all over the country, the initiative for this came from the medical professionals. All doctors are aware of the Hippocratic oath but a growing number of physicians have come to feel that the Hippocratic oath was written long before the advancements in bioethics and is inadequate to address the realities of the modern medical world.1 It makes no mention of such contemporary issues as the ethics of research or a doctor’s societal responsibilities. Doctors in Myanmar still believe in the spirit of the Hippocratic oath but is it still applicable in the current crisis that we face in Myanmar?
In India, in the Charaka Samhita, a sanskrit text on Indian traditional medicine, physicians could refuse to treat people who were not favoured by the king, which shows that oaths were a product of the sociocultural factors of the times they were created.2
Doctors in Myanmar decided to start the strike known as The Civil Disobedience Movement (CDM), and more than 80% of doctors got involved. They are not from political backgrounds but are committed to supporting the next generation in their struggle for democracy and feel unable to obey this illegitimate government.
Some doctors are collaborating with the private sector and non-government organisations to provide essential health care to people. Unfortunately, the military have detained thousands of medical professionals and volunteer staff. Many of the medical staff cannot stay in their homes and have to move from place to place to avoid being arrested by the military.
COVID-19 cases began to rise sharply in early June 2021 and there was a significant increase in the number of COVID-19 related mortalities. This is a catastrophic humanitarian crisis and the people of Myanmar are suffering because of the impact of both COVID-19 and the coup.
Military terrorists are using COVID-19 as a bioweapon, they are blocking the supply of medicines that are used to treat COVID-19, as well as taking away the oxygen supplies of the private and volunteer organisations. On 16 July, one private hospital in Myamar had to shut down their emergency department because the military had cut off the oxygen supply.
The Junta has stated in the newspaper ‘We have enough oxygen’ but this is untrue, they are blocking the supply of oxygen. Two colleagues of mine from medical school died in ITU at one of the government hospitals because of a lack of oxygen.
The people of Myanmar, including my family and relatives, are desperately searching for oxygen. On 13 July Yangon General Hospital was overwhelmed by desperate people needing oxygen treatment but the hospital didn’t have enough of a supply or enough staff. The police fired shots above the crowd to drive them away.
The healthcare system is at breaking point, some medical professionals are hiding in the jungle. Providing primary medical care is a real challenge.
Through webinars doctors in the UK, especially those from Myanmar, are giving moral support to their colleagues in Myanmar, and are helping by sharing their experience for the home management of COVID-19 and some common medical conditions. They are also trying to find ways to supply oxygen concentrators but are concerned that supplies might not reach the needy civilians and that doctors involved would be detained by the military.
Some Myanmar doctors here in the UK have significant feelings of guilt because as medical professionals we do not feel we are able to effectively support colleagues to provide health care for their communities back home.
Doctors in Myanmar are aware that the international community has expressed concern for our country. In supporting the CDM, they are caught between the duty of care they have for the wellbeing of the communities they serve and the need to make a stand for democracy and freedom in our country.
References
1. Tyson P. The Hippocratic oath today. 2001. https://www.pbs.org/wgbh/nova/article/hippocratic-oath-today (accessed 31 August 2021).
2. Indla V, Radhika MS. Hippocratic oath: losing relevance in today’s world? Indian J Psychiatry 2019; 61(Suppl 4): S773–S775.
Read further on the healthcare crisis in Myanmar on BJGP Life
The dream of universal healthcare in Myanmar becomes a nightmare.
Project Empathy. A response to the healthcare crisis in Myanmar.
Myanmar doctors under a military coup in the midst of the pandemic.
Featured images from Dr Jim Brockbank.
Jim Brockbank has retired from general practice. He continues in his role as a GP Appraiser and as an International RCGP Trainer for Myanmar.
Athird wave of COVID-19 is raging across Myanmar, the sick are being left to die in the streets or at home, smoke pours from crematorium chimneys, makeshift morgues are overflowing, two dead are put in one casket such is the shortage of coffins. Given the military’s crackdown on information it is difficult to obtain true figures on COVID-19 cases and deaths, but the evidence is in the streets.
It’s hard to understand the actions of a leadership that attacks doctors and nurses at the peak of a pandemic, but that is what is happening in Myanmar. Medics fear arrest or detention at a time when Myanmar needs them most.
The arrest of Dr Htar Htar Lin, the former head of the vaccination programme in Myanmar, has been previously discussed in this journal.2 In a breathtaking example of conceit and entrapment three doctors were arrested in July after they arrived at an apartment in Yangon to attend a severely breathless man, he proved to be a police officer feigning illness.3 The doctors were from a group who advise virus sufferers over the telephone how to breathe, how to use an oxygen concentrator, and which medicines to buy and how to administer them. Witnesses saw the doctors, handcuffed and bruised, being led away. Their covert clinic was raided, oxygen cylinders and PPE were seized. In addition to seizing oxygen cylinders it is reported that the Junta are blocking factories from re-filling people’s oxygen cylinders.3
In Yangon the security forces opened fire on civilians queuing in line for oxygen, and in Mandalay the military killed one civilian searching for oxygen. There have been reported incidents of patents with COVID-19 being refused admission to hospital.3 In August the number of people killed due to political violence surpassed 1000. Thousands more have been injured, and more than 3300 people remain in detention, including healthcare workers.4
The Junta has centralised all resources for providing medical aid including vaccines, oxygen, and medication. Testing for COVID-19 has plummeted and the vaccination programme has stalled, available data show that only about 6% of the population of 54 million have been fully vaccinated.5
The severe shortage of oxygen, medical equipment, and medication in cities across Myanmar has resulted in people hanging yellow and white flags outside their homes to signal that they need food or medicine, social media has been flooded with pleas for help.6
COVID-19 meets a weak and overwhelmed healthcare system
The crackdown on health care is hitting an already vulnerable system at a critical time. Before the coup Myanmar had 6.7 physicians per 10 000 people in 2018, significantly lower than the global average of 15.6.7 Despite limited resources the Myanmar healthcare system managed to cope with the virus last year, but the coup changed all that.
The National League for Democracy (NLD) recognised the need to improve the healthcare system, which resulted in The New National Health Plan for Myanmar 2017–21 being launched in March 2017 by Aung San Suu Kyi. This is where my own connection and commitment to Myanmar began, which has been previously discussed in this journal.8
In addition to coping with COVID-19 the healthcare system is struggling to provide general health care, and UNICEF has reported that about 600 000 newborn are not receiving essential care, a million children are missing out on routine immunisations, and more than 40 000 children are no longer getting treated for malnutrition.7 Pregnant women and other vulnerable groups face new obstacles in reaching essential care and basic services. Necessary acute, chronic, and preventive care for their communities is an immense challenge for healthcare providers.
Access to health care is particularly challenging in the rural areas and for the population of internally displaced people in the border regions. Over the last 3 months, around 2500 people have arrived in one locality where a group of doctors and nurses have set up medical facilities.
They additionally provided a quarantine centre where new arrivals could be isolated according to World Health Organization guidelines. Over a 4-week period they identified 60 COVID-19 cases and successfully managed three moderate-to-severe cases with oxygen saturation levels <93% in the makeshift COVID-19 inpatient centre. Healthcare staff can get further support and advice on social media from the Ministry of Health in the opposition National Unity Government (NUG), which is run by medics who are part of The Civil Disobedience Movement. COVID-19 test kits, PPE, and medical equipment is provided through donations.
COVID-19 cases are on the increase, there is delay in obtaining medical equipment and medication because of transport problems to these regions, let alone the thievery of the Junta, and a major constraint is that severe COVID-19 cases can’t be transferred to hospital because of lack of staff and people who are frightened to attend.
The call for civil disobedience has been stepped up
The dilemma of civil disobedience at a time of COVID-19 was discussed in this journal recently.9 The launch of a people’s defensive revolution by the president of the NUG on 7 September calling for the people of Myanmar to revolt against the Junta could escalate the conflict to a point where the healthcare system itself is dead and buried.10 A military coup coupled with a stricken healthcare system and a pandemic has already killed thousands, Myanmar could be left with no room to breathe.
The monitoring of how to continue to deliver support for healthcare workers in their commitment to deliver urgent, routine, and COVID-19-related health care to their communities will need to be doubled down. Solutions will need to be found regarding access to health care and to medical training.
Getting down to the facts
In a recent survey of 25 000 people who suffered from COVID-19, the NUG Ministry of Health compared data announced by the State Administration Council (SAC), representing the Junta.11 The death rate was 15% regardless of the place of death, five times higher than the 3.2% reported by SAC, which counted only hospital deaths. Thirty-four per cent of patients with suspected COVID-19 sought care online and 21% from home care services; only 5% received hospital care from government hospitals. Of all the responders, 25% received oxygen treatment. Most of the patients who were critically ill did not receive the necessary hospital care; 73% of deaths occurred at home, 17% of deaths occurred in government hospitals.
Frontline care in a ‘perfect storm’
Imagine trying to provide health care in these circumstances, not surprisingly doctors and nurses are overwhelmed. The reality is that the majority of patients with COVID-19, including people with severe disease, are staying home; they are either self-treating, or relying on care from local doctors and nurses operating in secret. Ducking and diving under cover, medication in short supply, and 73% of COVID-19 deaths occurring in the home — these are extraordinary challenges.
Cultural factors shape health-related beliefs and behaviours. There is a wrong assumption that available medicines for COVID-19 should be given to patients as early as possible, and the concept of ‘right patient at the right time with the right dose’ is stressed. Antivirals and antibody products can be very expensive, and ethical prescribing with clear discussion of benefits is encouraged. Clinicians need to be prepared for managing deterioration and death alongside the acute medical management plan. Severely ill patients need an explanation that hope that their treatment will help needs to be balanced with the fact that they are sick enough to die.
The concept of palliative care is new to doctors and nurses in Myanmar, and it is a step change to accept that palliative care is not ‘giving up’ but is active management for patients not responsive to curative treatment with the goal of achieving the best quality of life. This is a real challenge in the context of shortage of even basic medication including analgesics, anxiolytics, and corticosteroids.
Most nurses, who previously worked in the hierarchical system of government hospitals, have refused to return to work since the coup and many nurses now provide community level health care outside of hospitals in ‘pop-up’ clinics. Many nurses and student nurses find themselves the only healthcare provider in their village, a role for which they were never trained. They work with a lack of supplies and live under the constant fear of arrest, recently two nurses purchasing supplies of medication were arrested (Anonymous, personal communication, 2021).
On the government-run TV stations live arrest warrants are announced for nurses, and those who have been arrested have been paraded ‘confessing’ on prime-time evening television. Yet they continue, supporting their communities and their patients.
Continuing to deliver support for healthcare professionals
In all this doctors and nurses need help, and the UK health community response to the call for educational support from Myanmar colleagues has resulted in an impressive array of initiatives previously discussed in this journal.12
Regular webinars on COVID-19 for GPs are now taking place. Teaching topics include:
drug therapies in the management of COVID-19;
vaccines;
thromboprophylaxis in COVID-19;
impact of COVID-19 on non-communicable diseases (NCDs);
long COVID;
palliative care — end-of-life care, specific to COVID-19; and
roleplay in Burmese.
Recent funding has been approved for ‘strengthening the Myanmar GP service provision during the COVID-19 pandemic’ by the Foreign, Commonwealth and Development Office (FCDO). This will include small group education webinars, strategies to build personal resilience, and practical support for PPE, oxygen, and medication.
Myanmarclinicalguidance.com is a website established by the Royal College of Paediatrics and Child Health (RCPCH), it does not collect any user identifiable data and is low bandwidth for easy access. The site contains clinical guidelines and medical resources selected by experts for use by doctors, nurses, and others in Myanmar, and includes a course titled ‘COVID-19 primary care response in low resource settings’ with the following topics:
cover a guide to public health measures;
triage and management in primary care;
planning for healthcare delivery during the pandemic;
prevent the spread of COVID-19;
NCDs and COVID-19; and
mental health for the community during COVID-19.
The site also links to an increasing number of social-media-friendly videos, with Burmese narration and subtitles that give Burmese clinicians guidance on medical procedures and the general public advice on first aid.
The global health picture
‘Vaccines must be tools of protection, not politics’13
If the coup itself did not prompt concerted international efforts to resolve the humanitarian crisis, the public health implications certainly should. Myanmar borders India, China, and Thailand, and Myanmar is at risk of becoming a COVID-19 super-spreader. The United Nations (UN) special rapporteur for Myanmar has urged the security council to call for a ceasefire. It is reported that a ceasefire has been declared by the Junta for humanitarian aid, but nobody trusts them.
It is hoped that the UN Secretary General will seize the initiative and travel to Myanmar to negotiate a sustained halt to the conflict to allow a third party vaccination programme to be undertaken, in which humanitarian workers will be neither obstructed nor targeted. Engagement of the people of Myanmar will be a challenge in itself and public trust in COVID-19 vaccines and vaccination will be as essential as the effectiveness of the vaccines themselves. Let’s hope the military will accept international assistance to contain the coronavirus.
References
1. Amnesty International. Myanmar: military threatening health workers amid COVID-19 surge. 2021. https://www.amnesty.org.uk/press-releases/myanmar-military-threatening-health-workers-amid-covid-19-surge/ (accessed 16 Sep 2021).
2. Anonymous. Myanmar’s Director For Covid Vaccination Programme tests positive whilst in prison. 2021. https://bjgplife.com/2021/07/20/myanmars-director-for-covid-vaccination-programme-tests-positive-for-covid-whilst-in-prison (accessed 16 Sep 2021).
3. Insecurity Insight. Violence against or obstruction of health care in Myanmar. 2021. http://insecurityinsight.org/wp-content/uploads/2021/08/Violence-Against-Health-Care-in-Myanmar-February-July-2021-August-update.pdf (accessed 16 Sep 2021).
4. United Nations. Daily press briefing by the office of the spokesperson for the Secretary-General. 2021. https://www.un.org/press/en/2021/db210823.doc.htm (accessed 16 Sep 2021).
5. Our World in Data. Coronavirus (COVID-19) vaccinations. Myanmar: share of people vaccinated against COVID-19, Sep 11, 2021. 2021. https://ourworldindata.org/covid-vaccinations (accessed 16 Sep 2021).
6. Ratcliffe R. Myanmar could become Covid ‘super-spreader’ state, says UN expert. The Guardian 2021; 28 Jul: https://www.theguardian.com/world/2021/jul/28/myanmar-could-become-covid-super-spreader-state-says-un-expert (accessed 16 Sep 2021).
7. Gelineau K, Milko V. In Myanmar, the military and police declare war on medics. 2021. https://apnews.com/article/only-on-ap-myanmar-business-science-coronavirus-pandemic-3b4c3e6d711b5eac1209a2c8fd90b2b4 (accessed 16 Sep 2021).
8. Brockbank J. The dream of universal healthcare in Myanmar becomes a nightmare. 2021. https://bjgplife.com/2021/03/29/the-dream-of-universal-healthcare-in-myanmar-becomes-a-nightmare (accessed 16 Sep 2021).
9. Aung HM. The dilemma of civil disobedience at a time of COVID. 2021. https://bjgplife.com/2021/09/03/the-dilemma-of-civil-disobedience-at-a-time-of-covid-19 (accessed 16 Sep 2021).
10. Davies E. Myanmar shadow government calls for revolt against military rule. 2021. https://www.reuters.com/world/asia-pacific/myanmar-shadow-government-unveils-new-strategy-oppose-military-rule-2021-09-07 (accessed 16 Sep 2021).
11. Ministry of Health, National Unity Government. Assessment on COVID-19 during third wave by MOH, NUG. 2021. https://moh.nugmyanmar.org/assessment-covid-third-wave (accessed 16 Sep 2021).
12. Brockbank J. Project Empathy. A response to the healthcare crisis in Myanmar. 2021. https://bjgplife.com/2021/05/28/project-empathy-a-response-to-the-healthcare-crisis-in-myanmar (accessed 16 Sep 2021).
13. @UKUN_NewYork. #Myanmar: vaccines must be tools of protection, not politics. 2021. https://www.twitter.com/ukun_newyork/status/1427674683445481477 (accessed 16 Sep 2021).
Featured photo by Enchax Creative on Unsplash — ‘“Nothing burns like the cold so keep raising your frozen fingers”. The three-finger salute has become a symbol of resistance in protest and in art. Across the milk-tea nations, from Myanmar to Thailand to Hong Kong, the gesture represents global solidarity for democracy, defiance against tyranny, and the fight for freedom.’