 Dr Kulsum Janmohamed Rampling is a consultant in Public Health Medicine and General Practitioner. She works as a GP in Northamptonshire and as a menopause specialist.
Dr Kulsum Janmohamed Rampling is a consultant in Public Health Medicine and General Practitioner. She works as a GP in Northamptonshire and as a menopause specialist.
There’s something about menopause…
As GPs we aim to do our best for our patients. We spend time with them and listen to their stories, we go through their various documents, prescribe their medications, and try to ensure we “Do no harm”. A specialist writes to us asking us to prescribe a medication and we generally take heed of the advice and generate the prescription. We attend reputable GP-training events and feel confident that the training delivered will be up to date and relevant. And yet, there’s something about menopause where all this somehow falls apart.
HRT has faced backlash through the years. Older types have been associated with an increased risk of VTE.1 Furthermore, breast cancer risk was highlighted in the media after a non-statistically significant increase in risk was found in the WHI study in 2002, leading to headline news and the study being halted early.2 Little is mentioned around the decrease in risk that this same study (along with others) found for oestrogen only HRT taken in women who have had a total abdominal hysterectomy.3 This study and other studies’ findings of reduced colorectal cancer risk is rarely touched upon,4,5 and the fact that these women were generally older, and not the healthiest cohort in terms of smoking status and weight is largely glossed over.6 Little focus is given to the many benefits of HRT such as reduction in osteoporosis risk,7 type 2 diabetes risk,8 and risk of Alzheimer’s disease. 9,10 Then of course there is symptom management: the sweats, flushes, vaginal pain, emotional lability, anxiety… the brain fog that has caused high-functioning women to give up well paid jobs, the drop in libido that can become so intense that some women cannot even stand to be touched.
Then of course there is symptom management: the sweats, flushes, vaginal pain, emotional lability, anxiety… the brain fog that has caused high-functioning women to give up well paid jobs, the drop in libido that can become so intense that some women cannot even stand to be touched.
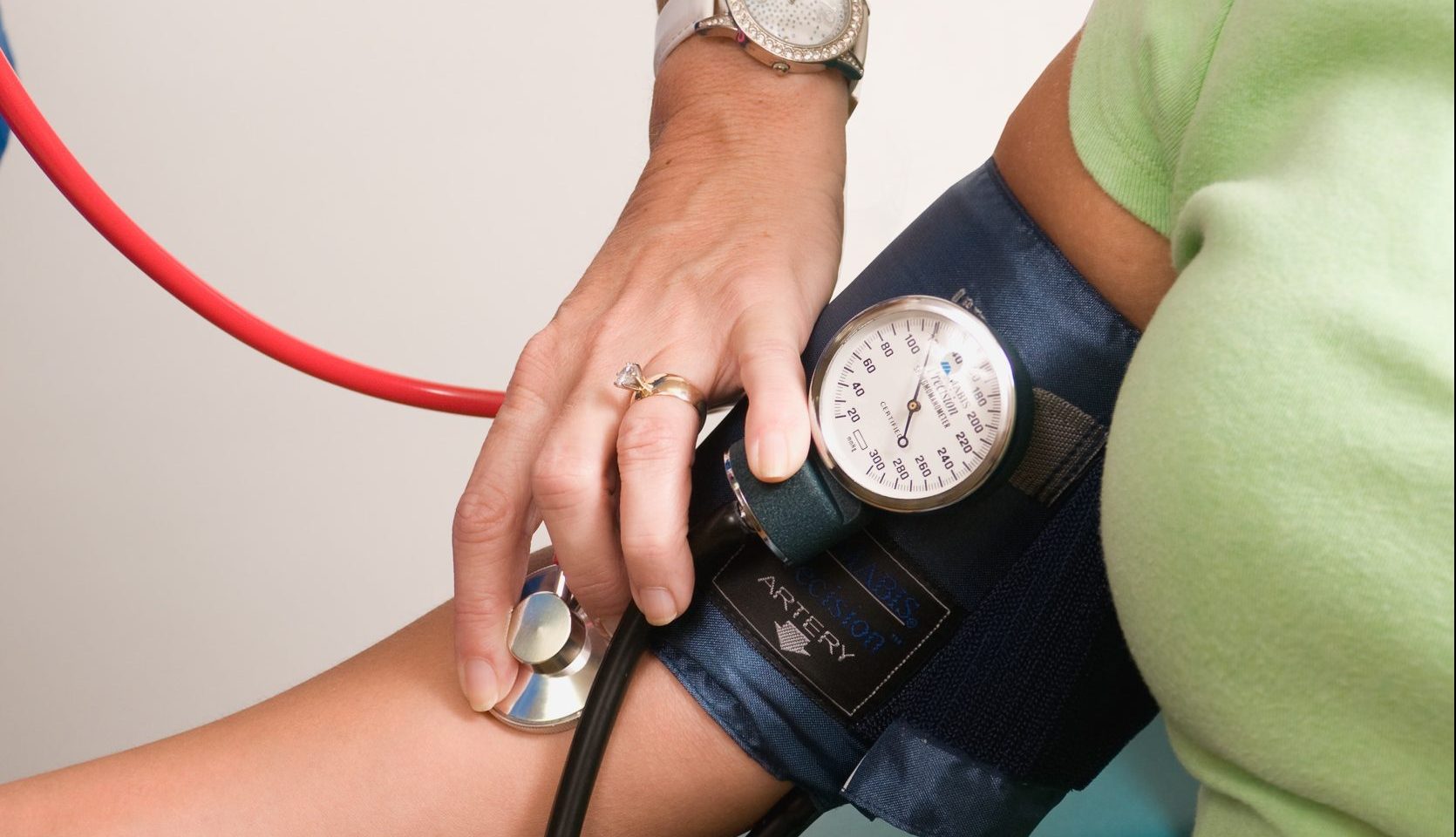
Over the years, advances in HRT have thankfully been made, and we have moved from hormones derived from pregnant mares’ urine to body identical hormones produced from yams. Studies have found that body identical HRT is associated with no increased risk of blood clot11,12 (and is unlikely to be associated with any increase in breast cancer risk13,14) and yet many doctors remain reluctant to prescribe this treatment to women with raised blood pressure. GPs are alarmed if menopause clinics issue a prescription without documenting a blood pressure reading in the clinic letter. As we all know, documenting blood pressure, and addressing hypertension is ‘Bread and butter’ medicine. However, nobody bats an eyelid when an endocrinologist recommends thyroid treatment to an individual without first documenting their blood pressure, so why is there a different attitude for modern-day HRT?
When a menopausal woman is so exhausted that she cannot exercise, cannot motivate herself to eat well and feels so negative about herself that she self-medicates with alcohol, is it little wonder that her prescribed ramipril is not adequately treating her hypertension? Shall we also wonder why our well-meant advice for her to diet and exercise is not taken up? Or shall we prescribe her some HRT, observe her sense of wellbeing and energy levels improve, and maybe even notice her blood pressure “magically” fall into the normal range.
In some respects, I am not surprised that attitudes around HRT have changed little among many doctors. I recently attended a reputable training course for GPs. I was feeling heartened that there was to be a focus on menopause and testosterone. Unfortunately, I sat disappointed as surprisingly inaccurate information was disseminated on this topic. It is therefore not entirely surprising when I listen to my GP colleagues expressing irritation when a menopause clinic letter requests a GP prescription for HRT including testosterone, which they do not feel comfortable prescribing.
Testosterone is not licenced for women in the UK, but this was not always the case. There used to be a licenced testosterone patch for women in the UK who had experienced a surgical menopause. This patch has since been discontinued, with “commercial reasons” (i.e. lack of profit) being cited as the cause.15
Menopause management, while its benefits have been largely ignored, belittled, or swept under the carpet, is a huge topic and treatment is so important, from symptom management to public health benefit.
When I turn to biology I am reminded that the ovaries produce three hormones and testosterone is one of them. The adrenal glands produce this hormone too but when the ovaries pack in there is a clear drop. Testosterone deficiency in women is associated with not just reduced libido but also mental and physical decline.16, 17 The arguments are persuasive for us as GPs to become competent and confident to prescribe this treatment in primary care for the good of our patients.18
Approximately 50% of our patients are females and menopause management is not rocket science. We would not feel uncomfortable prescribing anti-hypertension treatment, mental health treatment, arthritis treatment etc. Menopause management, while its benefits have been largely ignored, belittled, or swept under the carpet, is a huge topic and treatment is so important, from symptom management to public health benefit.
As GPs, it is our duty to question the reticence to prescribe, to think beyond what is being taught to us if it does not make sense, and to break the patriarchal mould that has been set long ago. Women’s health is important and it is our duty to be considered in our approach and to continually try to ensure that we achieve our promise to do no harm. When it comes to our ability to provide appropriate medical care, there’s always been something about menopause, and it needs to change.
References:
- Use of hormone replacement therapy and risk of venous thromboembolism: nested case-control studies using the QResearch and CPRD databases doi:10.1136/bmj.k4810
- Clark JH. A critique of Women’s Health Initiative Studies (2002-2006). Nucl Recept Signal. 2006 Oct 30;4:e023. doi: 10.1621/nrs.04023. PMID: 17088939; PMCID: PMC1630688.
- Stefanick ML, Anderson GL, Margolis KL, Hendrix SL, Rodabough RJ, Paskett ED, Lane DS, Hubbell FA, Assaf AR, Sarto GE, Schenken RS, Yasmeen S, Lessin L, Chlebowski RT; WHI Investigators. Effects of conjugated equine estrogens on breast cancer and mammography screening in postmenopausal women with hysterectomy. JAMA. 2006 Apr 12;295(14):1647-57. doi: 10.1001/jama.295.14.1647. PMID: 16609086.
- Nelson HD, Humphrey LL, Nygren P, Teutsch SM, Allan JD. Postmenopausal hormone replacement therapy: scientific review. JAMA. 2002 Aug 21;288(7):872-81. doi: 10.1001/jama.288.7.872. PMID: 12186605.
- Rennert G, Rennert HS, Pinchev M, Lavie O, Gruber SB. Use of hormone replacement therapy and the risk of colorectal cancer. J Clin Oncol. 2009 Sep 20;27(27):4542-7. doi: 10.1200/JCO.2009.22.0764. Epub 2009 Aug 24. PMID: 19704062; PMCID: PMC2754905.
- Anette Tønnes Pedersen, Bent Ottesen, Issues to debate on the Women’s Health Initiative (WHI) study. Epidemiology or randomized clinical trials—time out for hormone replacement therapy studies?, Human Reproduction, Volume 18, Issue 11, November 2003, Pages 2241–2244, https://doi.org/10.1093/humrep/deg435
- Gambacciani M, Levancini M. Hormone replacement therapy and the prevention of postmenopausal osteoporosis. Prz Menopauzalny. 2014 Sep;13(4):213-20. doi: 10.5114/pm.2014.44996. Epub 2014 Sep 9. PMID: 26327857; PMCID: PMC4520366.
- Franck Mauvais-Jarvis, JoAnn E. Manson, John C. Stevenson, Vivian A. Fonseca, Menopausal Hormone Therapy and Type 2 Diabetes Prevention: Evidence, Mechanisms, and Clinical Implications, Endocrine Reviews, Volume 38, Issue 3, 1 June 2017, Pages 173–188, https://doi.org/10.1210/er.2016-1146
- Depypere, H, Vergallo, A, Lemercier, P, et al. Menopausehormone therapy significantly alters pathophysiological biomarkers of Alzheimer’s disease. Alzheimer’s Dement. 2022; 1- 11. https://doi.org/10.1002/alz.12759
- Matyi JM, Rattinger GB, Schwartz S, Buhusi M, Tschanz JT. Lifetime estrogen exposure and cognition in late life: the Cache County Study. Menopause. 2019 Dec;26(12):1366-1374. doi: 10.1097/GME.0000000000001405. PMID: 31613825; PMCID: PMC7448538.
- Vinogradova Y, Coupland C, Hippisley-Cox J. Use of hormone replacement therapy and risk of venous thromboembolism: nested case-control studies using the QResearch and CPRD databases BMJ 2019; 364 :k4810 doi:10.1136/bmj.k4810
- Hamoda H, Panay N, Pedder H, Arya R, Savvas M. The British Menopause Society & Women’s Health Concern 2020 recommendations on hormone replacement therapy in menopausal women. Post Reproductive Health. 2020;26(4):181-209. doi:10.1177/2053369120957514
- Lewis PJ, HRT and breast cancer risk – progesterone vs. progestins,
BMJ 2019;367:l5928, https://www.bmj.com/content/367/bmj.l5928/rr-3https://doi.org/10.1136/bmj.l5928 - Stute P, Wildt L, Neulen J. The impact of micronized progesterone on breast cancer risk: a systematic review. Climacteric. 2018 Apr;21(2):111-122. doi: 10.1080/13697137.2017.1421925. Epub 2018 Jan 31. PMID: 29384406.
- https://writehealth.co.uk/testosterone-implants-available-in-the-uk/
- Rebecca Glaser and Constantine Dimitrakakis.Testosterone Implant Therapy in Women With and Without Breast Cancer: Rationale, Experience, Evidence.Androgens: Clinical Research and Therapeutics.Dec 2021.94-110.http://doi.org/10.1089/andro.2021.0003
- Glaser R, Dimitrakakis C. Testosterone therapy in women: myths and misconceptions. Maturitas. 2013 Mar;74(3):230-4. doi: 10.1016/j.maturitas.2013.01.003. Epub 2013 Feb 4. PMID: 23380529.
- Scott A, Newson, L. Should we be prescribing testosterone to perimenopausal and menopausal women? A guide to prescribing testosterone for women in primary care. British Journal of General Practice 2020; 70 (693): 203-204. DOI: 10.3399/bjgp20X709265




Thank goodness for a wholly sensible article on HRT and menopause! Thank you
I am sat in the waiting room at my doctors about to go in reading this …. I shall ask if they’ve read it depending on my treatment today. Yes it’s a menopause appt and taken 5 weeks to wait for a f2f. Ever hopeful for fair and educated treatment.
At last! Someone who gets it. Our GP’s need to get with the programme. Is it simply because, unlike diabetes or thyroid issues that affect both sexes, menopause is an exclusively female issue that there’s no interest?
Thank you for a current, real, helpful and informative article!
honestly comparing it to thyroid treatment in the Uk is not a good choice. An anyone who is hypothyroid will know gp’s in the Uk know very little about it and we are also treated awfully so yay to those of us who are hypothyroid and menopausal!