 Ayesha Siddqui is a sessional GP in Glasgow
Ayesha Siddqui is a sessional GP in Glasgow
Covid-19 has dramatically changed the way we provide healthcare to our patients. Telephone and video consultations have helped meet some of the challenges of reduced physical interaction, but come with their own limitations.
A middle- aged fit and healthy lady with no significant past medical history contacted the GP practice with symptoms of upper back/scapular area pain.* She reported a sudden onset pain in the entire right upper back area for a couple of days which wasn’t easing with over the counter analgesia. She did not report any fever or cough. She reported shallow breaths due to the pain. There was no history of injury or heavy lifting and there were no risk factors for venous thromboembolism. She was expecting to get some strong analgesia.
…she was in significant pain with no clear cause on history…
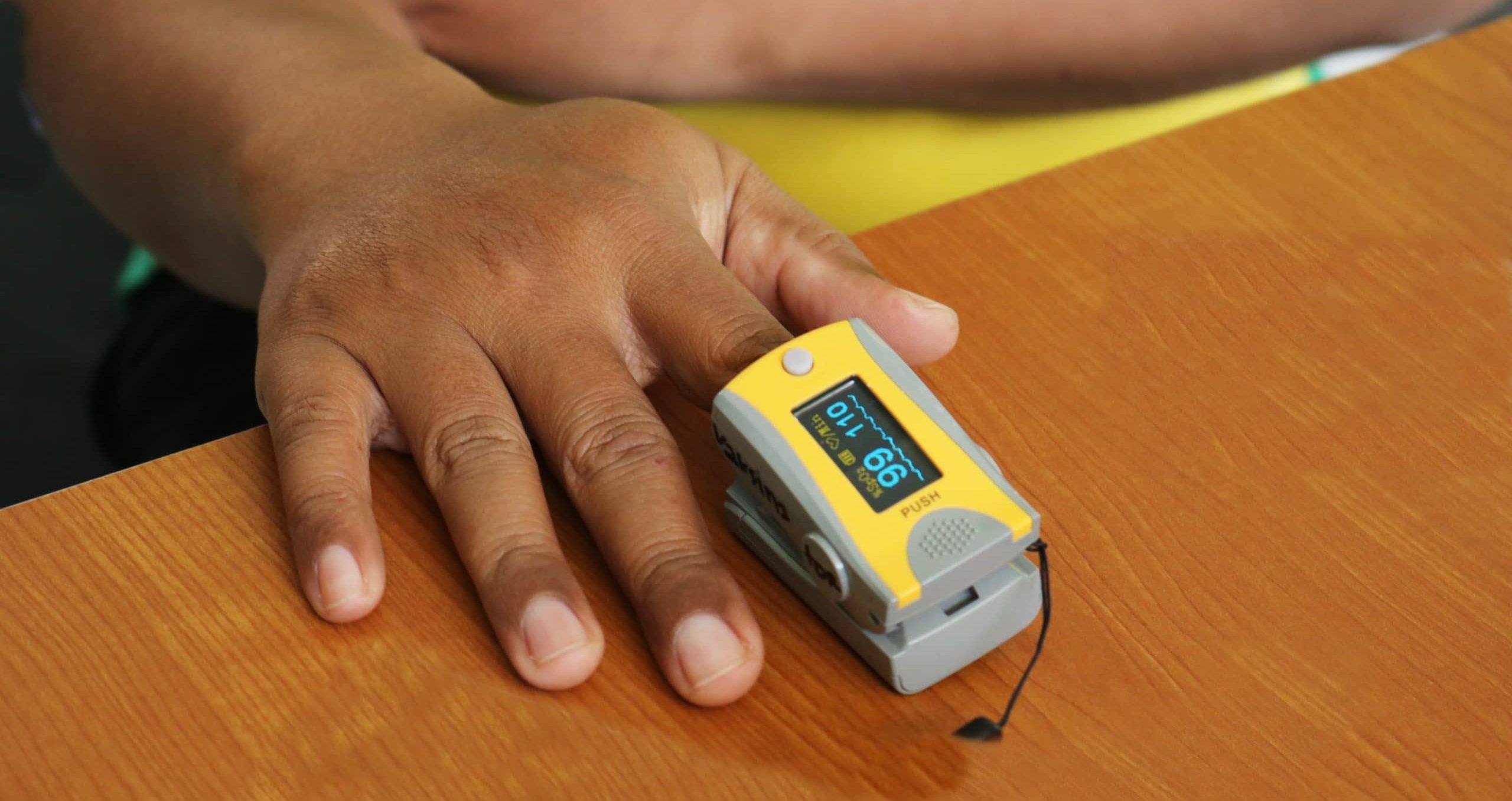
A couple of minutes into the telephone consultation, I realised that she was in significant pain with no clear cause on history. I arranged for her to attend the GP practice for a face to face consultation the same morning. On arrival, she was in her night clothes as the slightest of movement was exacerbating the pain. She was taking shallow breaths. The site of pain was from the nape of the neck and right shoulder down to the lower end of the shoulder blade and lower rib cage. She was afebrile, tachypnoeic at 32/minute and tachycardic at 132/minute. The blood pressure was 143/91 mmHg and oxygen saturation was 93% on air. The auscultatory chest examination revealed reduced air entry but she was taking shallow breaths due to pain. She had normal heart sounds.
Concerned about the possibility of a pneumothorax or pulmonary thromboembolism as a differential diagnosis (and much to the surprise of the patient who thought it was a pulled muscle and was expecting stronger painkillers), an urgent hospital review was arranged for the same day.
When she attended the acute assessment unit, she was found to have para-pneumonic pleural effusion on chest imaging and was in fast atrial fibrillation (AF). Computerised tomographic pulmonary angiography did not suggest venous thromboembolism. She received in patient care for 10 days and was discharged with a follow up chest radiograph at 6 weeks and an out-patient Holter monitor. She had a negative COVID-19 test.
She recovered uneventfully. A subsequent 24-hour tape showed that her AF had resolved and she has since stopped the anti-coagulants.
I feel that I could have easily mistaken her pain as musculoskeletal in origin over the telephone
On reflection, I feel that I could have easily mistaken her pain as musculoskeletal in origin over the telephone had I not been concerned about the intensity of her pain and had I not checked the vital signs when I examined her. This case has yet again highlighted the importance of going back to the basics if the diagnosis is unclear. It was a significant event with a positive outcome and a very important learning point for me.
With the Covid-19 pandemic and remote consulting, it is even more important to be vigilant for any cues and follow your gut instincts as a clinician, to ensure that potentially life threatening conditions are not missed. I am certain I am not alone in this realisation.
*With thanks to the patient who gave written consent to share this case.




This is a lesson for every GP. MSK symptoms can present any form but good caring observational listening GP picked up an unusual presentation acted upon timely and saved both patient and the GP.